Program At-A-Glance
Organization: Montefiore Medical Group
Description: Integrated care system providing primary, behavioral health, and specialty care to adults and children from low-income and diverse communities in the Bronx and lower Westchester County, New York.
Goal: Implement trauma-informed care throughout a large urban health outpatient care system.
Key Program Features: Training clinical and non-clinical staff on the impact of ACEs; soliciting patient input on clinic operations; screening for ACEs in adult and pediatric populations; and addressing employee trauma and burnout.
Montefiore Medical Group (Montefiore) is the largest health care provider in one of the poorest parts of the country, serving more than 300,000 people in the Bronx, New York. The Bronx leads New York State in premature deaths in people under age 65, with the leading causes including preventable illnesses such as heart disease, diabetes, and AIDS. Montefiore’s goal is to make care as easy, seamless, and comprehensive as possible, meeting patients in settings ranging from primary care clinics to specialty surgery centers and mobile medical vans. However, Montefiore recognizes that its patients face more than just logistical barriers to care. For Miguelina Germán, PhD, Assistant Director of the Pediatric Behavioral Health Integration Program at Montefiore Medical Group, the missing link between the care she provides and the persistently high rates of illness among her patients clearly comes down to pervasive trauma and a stressful living environment in an area with the highest poverty rate in New York City.
“For the Montefiore Medical Group, trauma is too often the elephant in the exam room and the reality of patients’ lives.”
In response, Montefiore has embraced trauma-informed care (TIC) as a way to treat the true, underlying causes of patient illness rather than its symptoms (missed appointments, poor medication adherence, health risk behaviors, etc.). Since its inception, Montefiore has been a leader in the field of physical and behavioral health integration, and has run a teaching program focused on the social origins of disease since 2005. Montefiore also operated the first HealthySteps program (an evidence-based pediatric primary care program committed to healthy early childhood development and effective parenting) available in the New York metropolitan area, which has now spread throughout the state. Recently, Germán and a cadre of other dedicated leaders at Montefiore have doubled down on their commitment to addressing trauma by working to expand adverse childhood experiences (ACEs) screening from birth through geriatrics at all primary care practices, and offering training on the impact of trauma and trauma-informed care practices to both clinical and non-clinical staff. These trainings cover how to identify and address common responses to trauma, the impacts of burnout and vicarious traumatization, how to promote team self-care, how to screen for ACEs, and the protocols for referring a patient to a behavioral health provider.
Germán hopes that the training convinces providers, and ultimately patients, that trauma-informed practices are the missing link between patient care and patients’ lives. Bridging the gap between the two, one patient and one staff member at a time, may offer the best hope for making the Bronx a healthier place to live and grow.
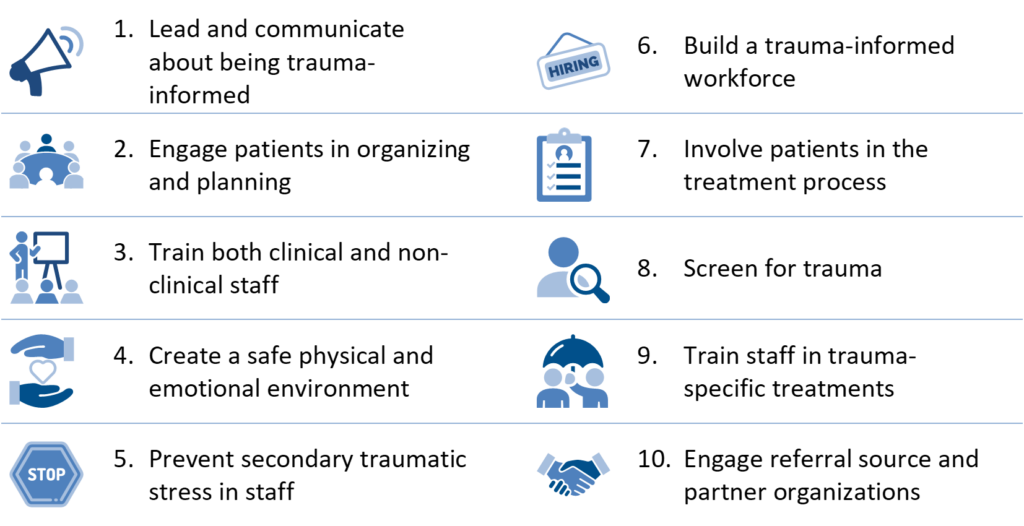
Ingredients of Trauma-Informed Care
Based on expert insights, the Center for Health Care Strategies (CHCS) compiled these core organizational and clinical elements to guide practitioners in pursuing trauma-informed care. Many of these ingredients are incorporated into Montefiore’s approach, with select features described below.
SOURCE: C. Menschner and A. Maul. Key Ingredients for Successful Trauma-Informed Care Implementation. Center for Health Care Strategies, April 2016.
Select Features of Montefiore’s Trauma-Informed Approach
Based on ingredients of trauma-informed care outlined above, following are select key aspects of Montefiore’s approach to addressing trauma.
 Leading and Communicating about the Transformation Process
Leading and Communicating about the Transformation Process
Andrew Racine, MD, PhD, Executive Director of Montefiore Medical Group, believes in the value of trauma-informed care and has dedicated a significant amount of resources to making Montefiore a trauma-informed system. With Racine’s approval, representatives from each primary care site (including primary care providers, nurses, operations managers and front desk staff) participated in four half-day training sessions on the following topics: (1) introduction to trauma-informed care; (2) manifestations of trauma; (3) ACEs screening; and (4) compassion fatigue, secondary trauma and developing team self-care plans. This training content was also disseminated to all primary care staff at Montefiore through role-specific online learning modules and through in-person trainings at the practices. The trainings were designed to create a common understanding of trauma and stress, develop empathy by teaching participants to take a different perspective, and overcome emotional reflexes by equipping staff with tactics to empathically manage tense situations.
 Engaging Patients in Organizational Planning
Engaging Patients in Organizational Planning
Patients, particularly those who have experienced trauma, play a large role in Montefiore’s Trauma-Informed Multidisciplinary Specialist (TIMS) team. TIMS is responsible for carrying out Montefiore’s trauma-informed initiatives, and ensuring that the changes are supported, sustainable, and ongoing. In addition to patient representatives, the team includes social workers, psychologists and psychiatrists, pediatricians, obstetricians, nurses, operations managers, support staff, and a patient representative. The team was instrumental in designing the content of the four half-day staff trainings described above. Of particular use were clinical vignettes (see below) — hypothetical difficult patient interaction scenarios used with staff as a learning tool on how to best respond to patients in a trauma-informed way.
Montefiore also created a patient experience questionnaire to help raise awareness about ACEs and the effects of toxic stress. The materials were designed in collaboration with the Patient Advisory Committee, a small group of patients with lived trauma experiences who have agreed to provide feedback on Montefiore’s trauma-informed transformation process.
Patient Vignette
Maria is 56 years old, and shares a two-bedroom apartment in the Bronx with her son, her partner, and their two young children. Maria arrives four hours late for her doctor’s appointment today. As the front desk representative, you explain to Maria that you will have to check with the doctor to see if she can be seen today. After checking with her PCP, you explain to Maria that the doctor is completely booked for the afternoon, and she can either be seen by her PCP first thing tomorrow morning, or by a nurse practitioner in two hours. You hand Maria the behavioral health screener as per clinic workflow. Maria becomes very agitated, and is yelling at you that she needs to be seen by a doctor today, and she cannot wait until the end of the day. She refuses to complete the behavioral health screener.
Why do you think the patient is acting like this? What is the #1 reason?
 Creating a Safe Physical and Emotional Environment
Creating a Safe Physical and Emotional Environment
At Montefiore, non-clinical staff are called Patient Service Representatives, and are trained in the principles of trauma-informed care. If a patient is agitated or upset, staff are taught how to de-escalate the situation. This results in a calmer, less intimidating waiting room experience.
Although patient waiting rooms vary across Montefiore’s network, an effort has been made to make signage more patient-friendly, and reduce the use of overhead loudspeakers and other disruptive noises.
 Preventing Secondary Traumatic Stress in Staff
Preventing Secondary Traumatic Stress in Staff
Montefiore’s network of 21 outpatient clinics are primarily located in underserved neighborhoods with high levels of violence and crime. In the past, events taking place outside clinic walls have weighed heavily on staff, many of whom live in the same communities where they work. In response, Montefiore created a team of behavioral health specialists, the Critical Incident Management Team, who are deployed to clinics within 24 hours of an incident in the community. After a recent shooting occurred outside of a Montefiore clinic, for example, the team visited staff the very next day. They debriefed the staff on the event, held support sessions, and offered referrals to counseling services for those who were interested. Staff say the debriefings make them feel cared for, and may help prevent post-traumatic stress disorder.
 Using Trauma-Informed Screening and Treatments
Using Trauma-Informed Screening and Treatments
As a national leader in physical and behavioral health integration, Montefiore practices already screened for mental health problems and psychosocial risk factors at most sites, starting at birth and continuing through late adulthood. In addition, at most of the clinics offering pediatric care, infants and their parents were universally screened using ACEs measure to assess children’s and parents’ exposure to trauma.
Montefiore’s goal is to expand ACEs screening to patients across the entire lifespan at all of its practices. To date, 11 of 13 pediatric practices, 6 of 13 internal medicine practices, and all 7 family medicine practices are screening for ACEs during the annual physical visit.
Next Steps for Trauma-Informed Care at Montefiore
In the future, Germán and her colleagues hope to spread ACEs screening and other trauma-informed practices beyond Montefiore Medical Group and throughout the entire Montefiore Health System, which serves hundreds of thousands of patients per year. If successful, Montefiore Health System would become one of the largest trauma-informed health systems in the country. Montefiore is also planning to hold a yearly training institute to teach other health care organizations across the country how to build a trauma-informed system of care. In leading by example, Montefiore hopes to inspire other large health systems to adopt trauma-informed care for the good of the complex populations they serve.
Trauma-Informed Care in Action Profile Series
This profile series features participants in Advancing Trauma-Informed Care, a national demonstration project designed to better understand how trauma-informed approaches can be practically implemented within the health care sector. LEARN MORE »