Program Snapshot
Name: Commonwealth Care Alliance Digital Health Pilot
Goal: Improve health care access, safety, and independence for patients with complex health needs.
Featured Services: Voice technology software that allows patients to schedule and pay for personal care attendants.
Target Population: Dually eligible Medicare-Medicaid enrollees with complex needs in Massachusetts.
In his roles as a physician and as a son caring for aging parents, John Loughnane, MD, saw that home-based, voice technology could be used for more than entertainment — it had the potential to improve health care access, safety, and independence for people with medical and psychosocial conditions. Loughnane is chief innovation officer for Commonwealth Care Alliance (CCA), a not-for-profit integrated Massachusetts health care organization that serves people with complex medical, behavioral health, and social needs. CCA members are dually eligible for Medicaid (MassHealth) and Medicare.A few years ago, as voice technology devices were becoming more widely used, one of Loughnane’s patients who had restricted mobility from a spinal cord injury and cancer began using a smart speaker to help him manage his home environment. Then Loughnane’s parents got a similar speaker system. Seeing the devices in action piqued his interest. “I thought there was a tremendous amount of power in voice [for patients with complex needs] if you learned how to scale it,” he says.
“I thought there was a tremendous amount of power in voice [for patients with complex needs] if you learned how to scale it.”
To explore that possibility, Loughnane and CCA embarked on the Center for Health Care Strategies’ Digital Health for Complex Populations: Pilot Challenge to study voice technology. The pilot focused on how to manage the scheduling and payment of personal care attendants (PCAs), tasks that CCA knew were often stressful for the people it serves.
The pilot began in 2016, aiming to enroll 100 CCA members. After the research team installed voice systems for the first 15 members and trained them on using the technology, some promising results emerged. People were able to communicate more easily with others through voice dialing or texting, which reduced their social isolation. Family or friends with similar devices could use a “drop-in” feature to stay in touch.
However, over time, several barriers became evident and ultimately led to discontinuing the initial pilot. Although the first effort did not work out, it gave the team valuable insights into how to deploy voice technologies and develop tools that align better with what people will use as part of their home-based care.
“What was supposed to be a pilot was really user acceptance testing between us and our patients about the potential of voice,” Loughnane says. After talking with participants and re-examining the identified barriers, study goals, and implementation, a new pilot was created and is now moving forward.
COMPLEX CARE INNOVATION IN ACTION
This profile is part of an ongoing series from CHCS exploring strategies for enhancing care for individuals with complex health and social needs within a diverse range of delivery system, payment, and geographic environments. LEARN MORE »
Analyzing Barriers
One difficulty encountered was that the initial pilot used Amazon Alexa voice technology with Echo Dot speakers. Because the hardware was chosen before more advanced models were available, the devices underperformed in sound quality and voice recognition. That was especially troublesome for people who had weak or soft voices due to respirator use or other conditions. Speaker quality was also a problem for those who spoke with strong accents and those with impaired hearing. In addition, some people could not take part in the pilot because the Alexa system only recognizes English and CCA serves many people with Hispanic and Creole backgrounds.
The initial pilot was a useful failure because it gave the team important insights into using voice technology to help those with complex medical and social needs and disabilities.
Setting up the system and devices, and getting them to run reliably, was time-consuming for both the team and the participants. CCA members needed to have a smartphone, working computer, and Amazon account to use the system in their homes, where Wi-Fi access was sometimes spotty. Set-up visits ran longer than foreseen and extra time was often needed to troubleshoot problems afterwards.
Participants and researchers had differing expectations about the pilot experience. While the team understood that a pilot system was a work-in-progress that would hit snags, they had not anticipated that participants would expect the technology to work smoothly from the beginning. According to the team, some members found these problems frustrating, and the devices were removed from their homes.
The team also discovered that, while stressful, the participants did not perceive managing PCA schedules and payments to be a significant problem. Many were satisfied using calendars or spreadsheets for those tasks. Instead, they valued the voice technology for providing other features that the team had not anticipated, such as playing music or turning lights on and off. The pilot could not investigate other uses for the voice system because the grant was confined to PCA issues. The program ended in January 2018.
Although the initial pilot fell short in several ways, it was a useful failure because it gave the team important insights into using voice technology to help those with complex medical and social needs and disabilities. From that learning experience, the CCA researchers developed a new pilot, which launched in October 2018.
Engaging Participants
When the team asked Lea Ann Markunis, of Framingham, Massachusetts, if she would be willing to try a voice-assisted system, she readily agreed. Markunis, who is 57, has diabetes, thyroid disease, shortness of breath, and asthma. Her left leg is amputated below the knee, so she uses a wheelchair.
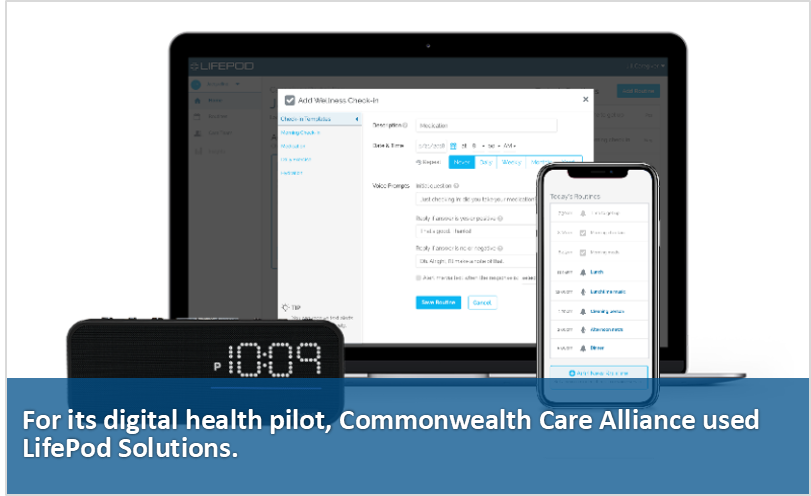
She was one of 55 participants in the first group of the new pilot. It uses voice-first software, a web portal interface, and a speaker device from LifePod Solutions, a voice services provider. The software is known as “proactive voice” because the system automatically communicates programmed messages directly to users, with eight to 12 daily reminders. It also does not need a prompting word or phrase, such as “Alexa,” or “Hey, Google,” for users to give a command or ask a question. The team noted this “proactive voice” system design significantly increases the frequency of participant use over a “passive” voice system.
Questions used in communicating to the participants are individualized for each person. For example, people who have recently had surgery might be asked if there is any redness around their surgical sites. Depending on the person’s response, the voice technology can then suggest a next step or offer to contact the person’s care manager or health care provider. In the future, Loughnane envisions expanding the programmed questions for a broader audience, such as asking users if they have had their flu shots — and, if needed, helping them to schedule those immunizations.
Markunis lives in a one-bedroom apartment and talks with her voice device throughout the day, every day. “It comes on with, ‘Lea Ann, did you take your medicine this morning?’ Or, ‘Don’t forget to eat your breakfast,’” she says. “It keeps me on track.” She knows the system is not a real person, but laughs about how it “gets an attitude” if she does not respond to its questions right away.
She receives messages telling her to drink more water, as well as reminding her to take her insulin or to eat regularly. The system also issues weather reports and entertains her with jokes. Markunis loves Polish music, so she asked the team to add it in. She was not the only one in her home who was delighted when that happened. “My parakeet would sing along and dance with the music,” she says. When the device was removed for two weeks because it was not working right, “this house was so quiet, I was lost without it,” she says.
Designing for Success
Although those dually eligible for Medicare and Medicaid may have limited incomes, many are tech-savvy.
Some people CCA serves, particularly elderly members, may live alone or spend long stretches of the day without human companionship. Voice technology helps them socially as well as medically.
The CCA team avoids taking a one-size-fits-all approach to creating a system. They think it is important to talk with the users, find out their needs and wants, and create the voice program that will be the right fit for each person.
The set-up process for the second pilot has gone more smoothly than it did for the first. Hardware and software can be adjusted to work better with each member’s voice characteristics or competing sounds from TVs and other noises in the home. The team also sets expectations with participants that the system might not function perfectly. Through the original pilot, “We learned how to [support] patients through technological challenges,” says Loughnane. “Almost none of the LifePods we have set up have come back and we have had a much better uptake rate once we have them out there.”
If and when the research supposition that voice technology will decrease clinical encounters is validated, the team intends to add more people to the pilot. Outcomes, such as fewer emergency department visits, will then be evaluated by CCA based on correlative trends.
Advice to Others
“We learned how to [support] patients through technological challenges. Almost none of the LifePods we have set up have come back and we have had a much better uptake rate once we have them out there.”
In spite of its promise, the growing trend toward making voice technology more accessible is also bringing challenges to health care organizations, planners, and designers. According to the CCA team, the future of voice technology use for people with complex medical and psychosocial conditions will depend on the results of more research and field testing of systems and devices. They advise others who are looking to try voice approaches to start with a small project, learn about how the devices can be tailored to individuals’ needs and preferences, and then establish goals.
Loughnane recommends testing the technology with a sampling of prospective users before creating a pilot, and spending time to pick partners carefully. “We had very supportive, thoughtful people working with us on both of the pilots,” he says.
CCA Digital Health Pilot Lessons
 Involved Participants to Identify Needs and Preferences
Involved Participants to Identify Needs and Preferences
- Don’t assume how participants will use the system. Ask potential users how they would like voice technology to help them.
- Create a consumer engagement panel to participate throughout the process.
Take Time to Identify the Right Voice Technology
- Develop technology well enough for successful use before giving to participants, even in a pilot.
- Start with a small feasibility round. Be mindful of which devices may have become outmoded by the time the pilot launches.
- Design technology to have value for everyday activities beyond medical or caregiving support.
- Choose a device with good sound quality for music and voice. It should be designed to fit on a coffee table so it doesn’t compete with furniture or medical equipment for space or power.
- Reminders may be more effective when they are given to participants on a schedule, without the user needing to prompt the device.
Provide Ample Support
- Make personal visits to set up the voice system and train participants. The researchers found that manuals and other written resources were not effective substitutes for in-person setup and training.
- Use a checklist for items to cover in the setup visit. Allow sufficient staff time for visits.
- After setup, have support help available so participants can get immediate answers to questions. Check in regularly with people who are using the technology.
Health plans and payers will need to develop approaches for identifying who could benefit from voice applications, and then establish implementation and payment strategies. The CCA team advises thinking about the process to be used, scalability, outcome measures, and the financial elements needed for success from the beginning.
CCA is continuing to expand its digital health pilot to reach 50 participants. Reaching that level will enable them to learn what is needed to scale up the program, and what it will cost. The team acknowledged, when expanding the program beyond CCA, that reimbursement from health plans will depend on determining how voice technologies can improve health, if those benefits can be quantified, and if they can be shown to decrease costs. Even though there is no clear payment path yet for voice-assisted services, many people with complex medical and psychosocial conditions find the technology empowering.
Author Robin Warshaw is an award-winning writer who focuses on medicine, social issues, and health care.
About the Center for Health Care Strategies
The Center for Health Care Strategies (CHCS) is a nonprofit policy center dedicated to improving the health of low-income Americans. It works with state and federal agencies, health plans, providers, and community-based organizations to develop innovative programs that better serve people with complex and high-cost health care needs. To learn more, visit www.chcs.org.
About the Complex Care Innovation Lab
Commonwealth Care Alliance is part of the Complex Care Innovation Lab (CCIL), a national initiative led by CHCS through support from Kaiser Permanente Community Health and the Robert Wood Johnson Foundation. Since 2013, CCIL has brought together leading innovators from across the country who are focused on improving care and outcomes for low-income individuals with complex medical and social needs. For more information, visit www.chcs.org/innovation-lab/.




